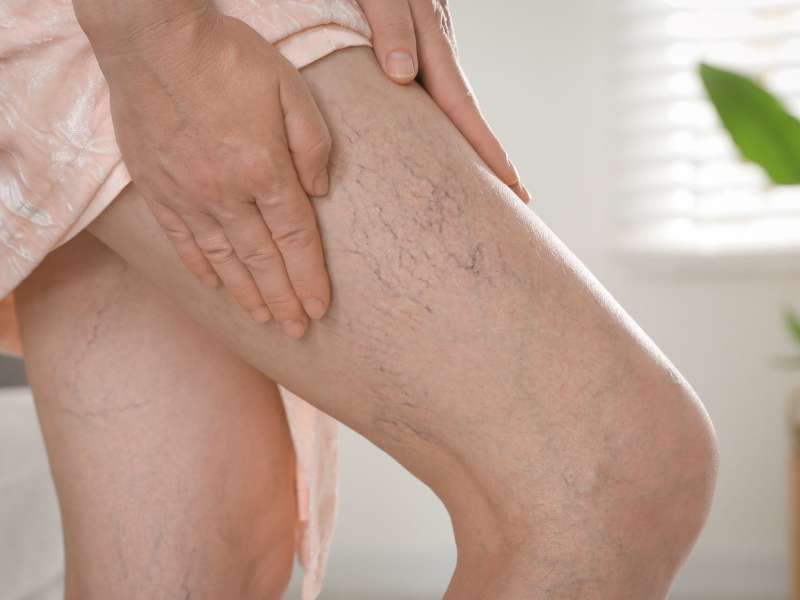
Does menopause cause varicose veins? It’s a question many Australian women ask themselves as they enter their golden years.
Studies have shown that varicose veins are common among female senior citizens. These large veins, often seen behind the legs, are often dark blue or purplish and may become prominent over time. This vascular disorder develops when damaged or compromised valves cause blood to accumulate in the veins. Instead of flowing back to the heart, the blood settles in the legs, making the varicose veins look prominent.
As a specialist Gold Coast menopause clinic serving Australian women since 2021, we understand varicose veins can be frustrating. That’s why we aim to help menopausal women navigate the challenges of midlife and successfully overcome this vascular disorder.
This blog explains why varicose veins develop during menopause and how to treat them, offering timely insights and information to help you enjoy your golden years and beyond.
Varicose Veins Defined
Varicose veins are swollen, enlarged blood vessels that develop beneath the skin’s surface. These blue or purple vessels often appear in the legs, feet, and ankles. Although varicose veins may cause discomfort or itching, they aren’t a serious health risk for many menopausal women. However, they can lead to serious health conditions, such as blood clots.
Women are more likely to develop varicose veins than men due to hormonal, bodily, and reproductive factors. Pregnant women experience increased blood volume and hormonal shifts, increasing pressure on leg veins.
The common symptoms of varicose vein development among menopausal and menopausal women include:
- A sensation of heavy or aching legs, especially after prolonged standing.
- Visible, bulging rope-like veins on the legs.
- Swelling in the feet or the ankles.
- Discolouration or dryness of the skin.
- Pelvic pressure or discomfort.
- Itching, throbbing, or burning sensations around the veins.
If you’ve been experiencing these symptoms, we strongly recommend consulting your women’s health doctor on the Gold Coast who can offer personalised advice for your situation.
What Are The Causes and Risk Factors of Varicose Veins?
Weakened blood vessel walls can lead to varicose veins. Increased blood pressure in the veins causes the veins to expand and become more prominent. Compromised valve function causes blood to pool and veins to swell and bulge.
The risk factors of varicose veins include:
- Age: Advanced age can compromise vein wall and valve function, causing veins to stiffen.
- Hormones: Progesterone and oestrogen affect vascular elasticity and allow vein walls to stretch when a woman goes through pregnancy, takes a birth control pill, or reaches menopause.
- Family history: Women with a family history of varicose veins can inherit this vascular disorder.
- Lifestyle: Prolonged standing or sitting can compromise circulation and cause varicose veins.
- Tobacco use: Women who use tobacco are more likely to develop varicose veins.
- Excess weight: Overweight women often experience higher pressure on blood vessels and experience varicose vein formation.
The Connection Between Menopause and Varicose Veins
As an established online women’s health service on the Gold Coast, we often remind our patients that hormonal shifts during menopause can lead to physiological changes, such as mood swings, hot flashes, and night sweats. These hormonal fluctuations can also affect the resilience and elasticity of blood vessel walls.
Diminishing oestrogen levels can affect those of nitric oxide, a molecule that helps blood vessels widen and remain flexible. Lower nitric oxide levels make veins less responsive to blood flow, leading to pooling and the development of varicose veins in the lower leg area.
On the other hand, progesterone helps blood vessels relax and improve circulation. Hormonal shifts during menopause can cause veins to stiffen and change in structure. Some studies have shown that these shifts can affect the vein health of menopausal women. Other findings have linked menopause to slower circulation and an increased risk of blood clotting, which both can lead to the development of varicose veins.
Perimenopause and Initial Vascular Changes
Some women experience physical changes during perimenopause—the critical transition period before menopause. Hormonal levels shift unexpectedly and affect many body parts, including the vascular system.
Engorged blue blood vessels appearing on the legs or chest are an early manifestation of varicose veins. Thinning, reduced skin fat tissues make these veins more prominent.
Some perimenopausal women experience leg swelling, especially in the late afternoons or early evenings. Although occasional swelling is a normal part of ageing, persistent soreness and extreme vascular changes may require urgent medical attention. At Her Medical, our established general practitioners can offer tailored solutions for vascular discomfort relief, improving your long-term health and quality of life.
Risk Factors for Varicose Veins During Menopause
Several risk factors can increase the likelihood of varicose veins during menopause, including:
- Multiple pregnancies and circulatory issues: These factors can increase the risk of menopausal varicose veins because they place repeated, long-term stress on the veins. Each pregnancy increases abdominal pressure, causing reduced blood flow from the lower limbs and weakening the veins over time.
- Natural vascular ageing: Weaker vein walls during menopause can lead to poor closure or vein valves and blood pooling, causing varicose veins to develop. Natural vascular ageing can also lead to poor circulation and worsen the situation.
- Weight gain and physical inactivity: Extra abdominal weight can increase pressure on pelvic and leg veins, impeding circulation back to the heart and leading to varicose vein formation. Lack of physical activity also slows down blood flow and increases the likelihood of valve failure.
- Hormone replacement therapy (HRT): HRT can influence hormone levels, vein wall properties, and circulation, contributing indirectly to conditions that can develop varicose veins in Australian women in their 50s or older. If you’re considering HRT, consult a reputable general practitioner on the Gold Coast who can provide you with tailored advice and insights.
Varicose Vein Management and Treatment Options
Menopausal women can successfully manage their varicose veins by following these recommendations:
- Regular exercise: Regular exercise, such as walking, swimming, yoga, and other leg-strengthening movements, improves blood flow, strengthens the muscles, and makes the veins more elastic. A healthy weight also significantly lessens strain on the veins.
- No prolonged sitting or standing: Take short, frequent breaks when sitting or standing for extended periods to increase blood flow and prevent blood pooling.
- Avoiding smoking and drinking alcohol: Avoiding tobacco and alcohol during menopause can improve vein strength, vascular health, and circulation, reducing the severity or likelihood of varicose veins.
- Medical treatment: Depending on your situation, your physician may recommend wearing compression stockings, injecting a special liquid or foam medication into the veins, or undergoing vein stripping, laser therapy, or endovenous ablation surgery. At Her Medical, we consider each patient’s lifestyle, preference, and past medical history when recommending the appropriate treatment plan.
Frequently Asked Questions (FAQs)
Why are varicose veins more common among menopausal women?
Fluctuating oestrogen and progesterone levels can influence circulation and vein strength, leading to varicose vein formation in midlife.
Can varicose veins naturally disappear?
Unfortunately, varicose veins do not naturally disappear. However, women can successfully manage them through healthy lifestyle habits and the prescribed treatment options.
What treatments are available for varicose veins?
Treatment alternatives include compression stockings, lifestyle changes, sclerotherapy, laser therapy, and endovenous ablation. Discussing your options with a trusted general practitioner often leads to successful long-term outcomes.
Conclusion
Varicose veins in midlife are a common result of hormonal shifts, natural vascular ageing, and lifestyle factors. Although they can be uncomfortable and make women more conscious about their appearance, they can successfully manage or reduce varicose vein symptoms through healthy lifestyle habits and effective medical treatments.
Discussing your situation with a trusted women’s doctor on the Gold Coast provides guidance and comfort and ensures optimal, long-term health and well-being. At Her Medical, we offer tailored solutions that can help you enjoy life in your golden years and beyond. Book an appointment today to speak with one of our general practitioners.